HIV Vaccine
Dedicated to the Pursuit of an Elusive Achievement
The human immunodeficiency virus, also known as HIV, is a retrovirus. If this human immunodeficiency virus goes untreated, it can lead to AIDS (acquired immunodeficiency syndrome). There are currently about 36.9 million individuals living with HIV worldwide, which is a major threat to public health, economic development, and cultural stability worldwide. One of the most effective ways to prevent many viruses is through the use of vaccines, which can be used to boost your immune system and prevent serious and life-threatening diseases. Due to the nature of HIV to rapidly mutate there are many kinds of HIV viruses circulating in a population that a vaccine has to be broadly effective for. Despite this challenge, several researchers across the globe are attempting to create a broadly neutralizing vaccine to address HIV, including Rama Rao Amara, PhD.

Rama Amara, PhD
Amara is a Professor at Emory University based in the Department of Microbiology and Immunology at the Yerkes National Primate Research Center with affiliation with the Emory Vaccine Center. His lab works on developing vaccines for infectious diseases and developing immunotherapies, with a major focus on developing novel prophylactic vaccines and therapy approaches to control HIV. For HIV research, his lab has developed two technologies: Trimeric Immunogen for HIV-1 Vaccination, and HIV-1 Clade C Protein Immunogen as HIV-1 Vaccine.
HIV is a virus that infects human CD4 cells. CD4 cells, or T cells, are white blood cells that are important for fighting infections and maintaining the body’s immune system. There are two types of T cells: the helper cells and the killer cells. The role of helper T-cells is to stimulate B-cells to make antibodies that are needed to fight infections. Killer T-cells are important for their role in directly killing cells that have already been infected by a foreign invader. HIV has the ability to delete helper T cells, which causes the infected individual's immune systems to become weak in response to viruses. This is known as immunodeficiency, and it can lead to the slow death of an HIV-infected individual.
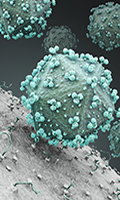
HIV Virus
Traditional therapy for controlling HIV-1 infection in humans involves antiretroviral therapy (ART). Although this treatment form has proven to be very effective, it has the disadvantage that it must be taken regularly and daily. Missing doses of antiretroviral therapy can impact the effectiveness of the therapy. Additionally, lifelong treatment also results in lifelong medical costs, which is not always accessible and possible for everyone who may be in need of HIV treatment. An HIV vaccine could be the solution to these issues of treatment adherence and cost. Vaccines typically provide longer-lasting protection from viruses such as HIV, and they eliminate the necessity of treatment adherence. Vaccines, in comparison with lifelong treatment regimens, are also more likely to be cost-effective.
Current attempts to produce viral vaccines focus on inducing neutralizing antibodies which inhibit viral entry into target cells. It has been very difficult to generate a vaccine that will induce a broadly neutralizing antibody, especially given the highly mutative status of HIV that has generated many variants of the virus. However, there are other types of antibodies, non-neutralizing antibodies, that do not block the infection but still provide protection. Once the virus gets into the infected individual’s cells, these non-neutralizing antibodies can clear the infected cells. The good thing about non-neutralizing antibodies is that they can be broadly cross-reactive and can potentially address more variants.

For the HIV-1 Clade C Protein Immunogen as HIV-1 Vaccine, Amara’s lab adopted structure and sequence guided strategies to develop a novel Clade C immunogen which can induce antibodies with neutralizing and other anti-viral properties. Additionally, for the Trimeric Immunogen for HIV-1 Vaccination, Amara’s lab also found a trimeric gp120 immunogen for HIV vaccine. This immunogen is able to promote strong, broadly cross-reactive V1V2 antibody responses in vivo. The ability to generate such cross-reactive antibodies suggests it has great potential as a vaccine antigen.
For the HIV vaccines in Amara’s lab, this research has completed two preclinical studies in nonhuman primates that proved protection for the simian immunodeficiency viruses, which is monkey-hosted HIV virus. The next step for this research is to finish preclinical development and plan clinical development.
"The potential for a vaccine that can address such a devastating, highly mutative disease is exciting," says Rajsekhar Guddneppanavar, assistant director of licensing with Emory's Office of Technology Transfer.
For additional information on Emory’s HIV/AIDS research please visit this website page.Techids: 17220, 20038
Read our technology brief for Trimeric Immunogen for HIV-1 Vaccination
Read our technology brief for HIV-1 Clade C Protein Immunogen as HIV-1 Vaccine